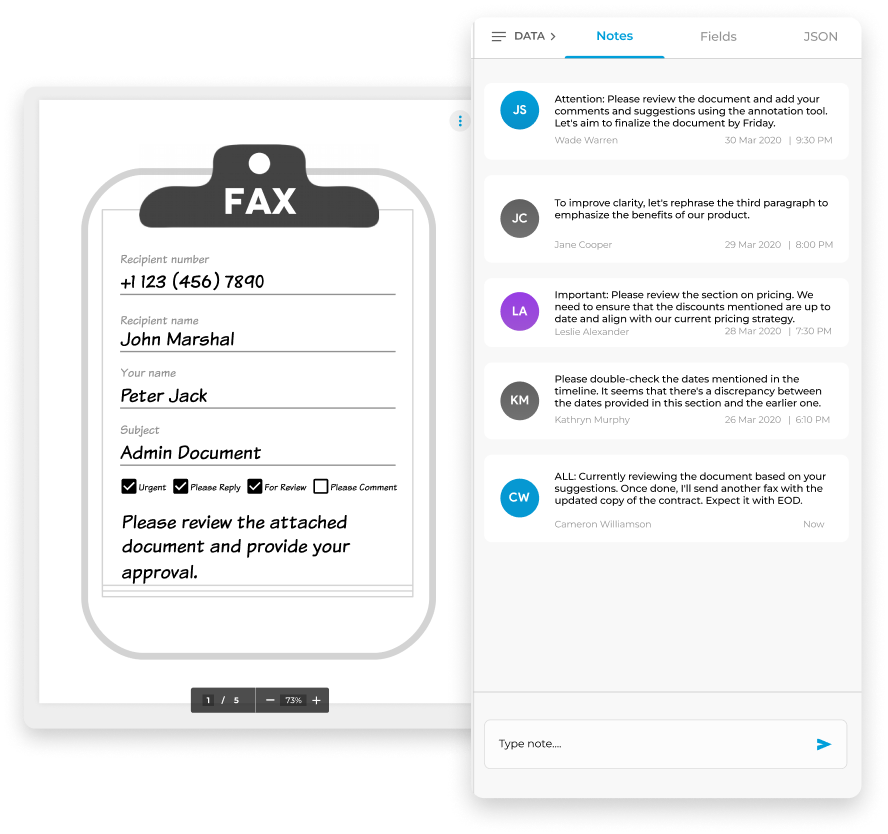
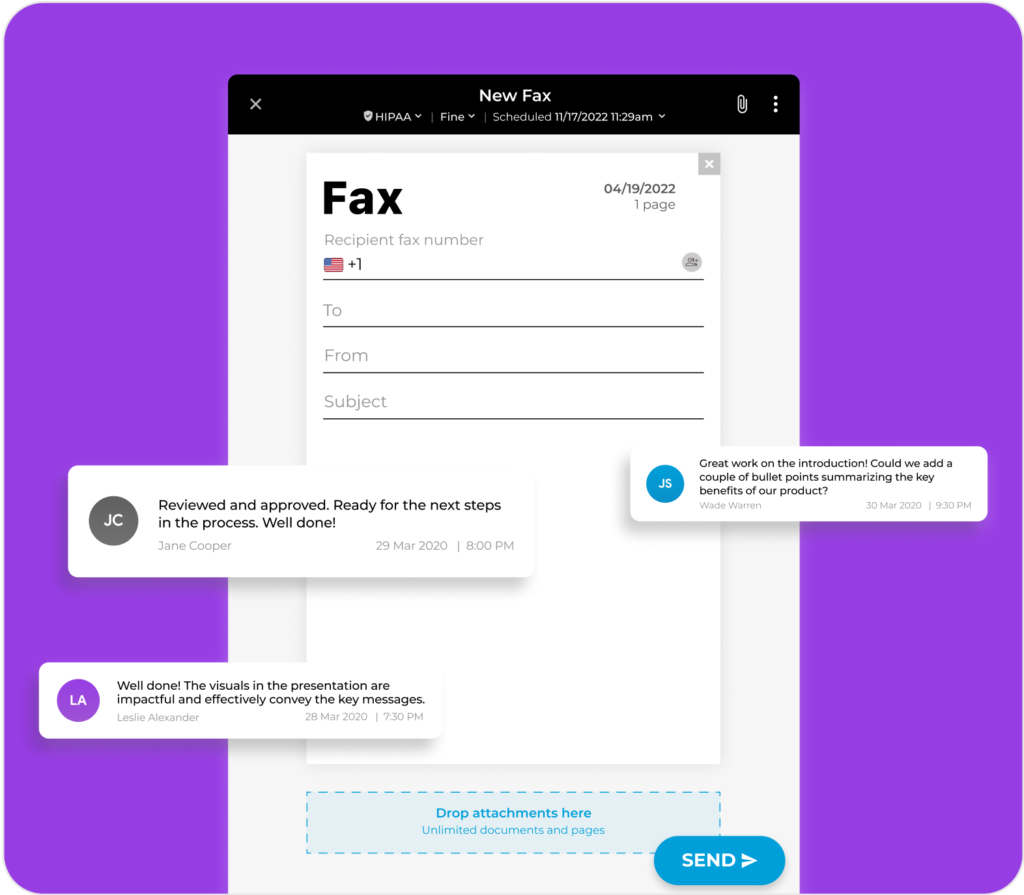
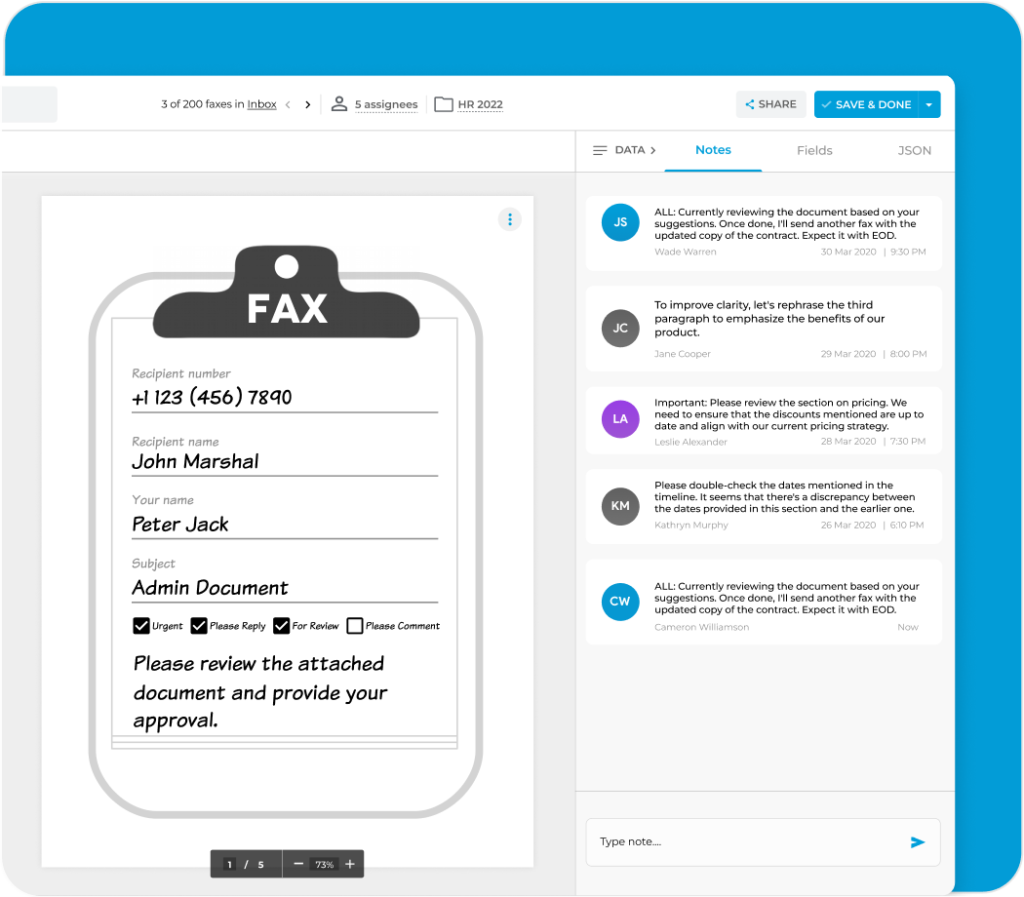
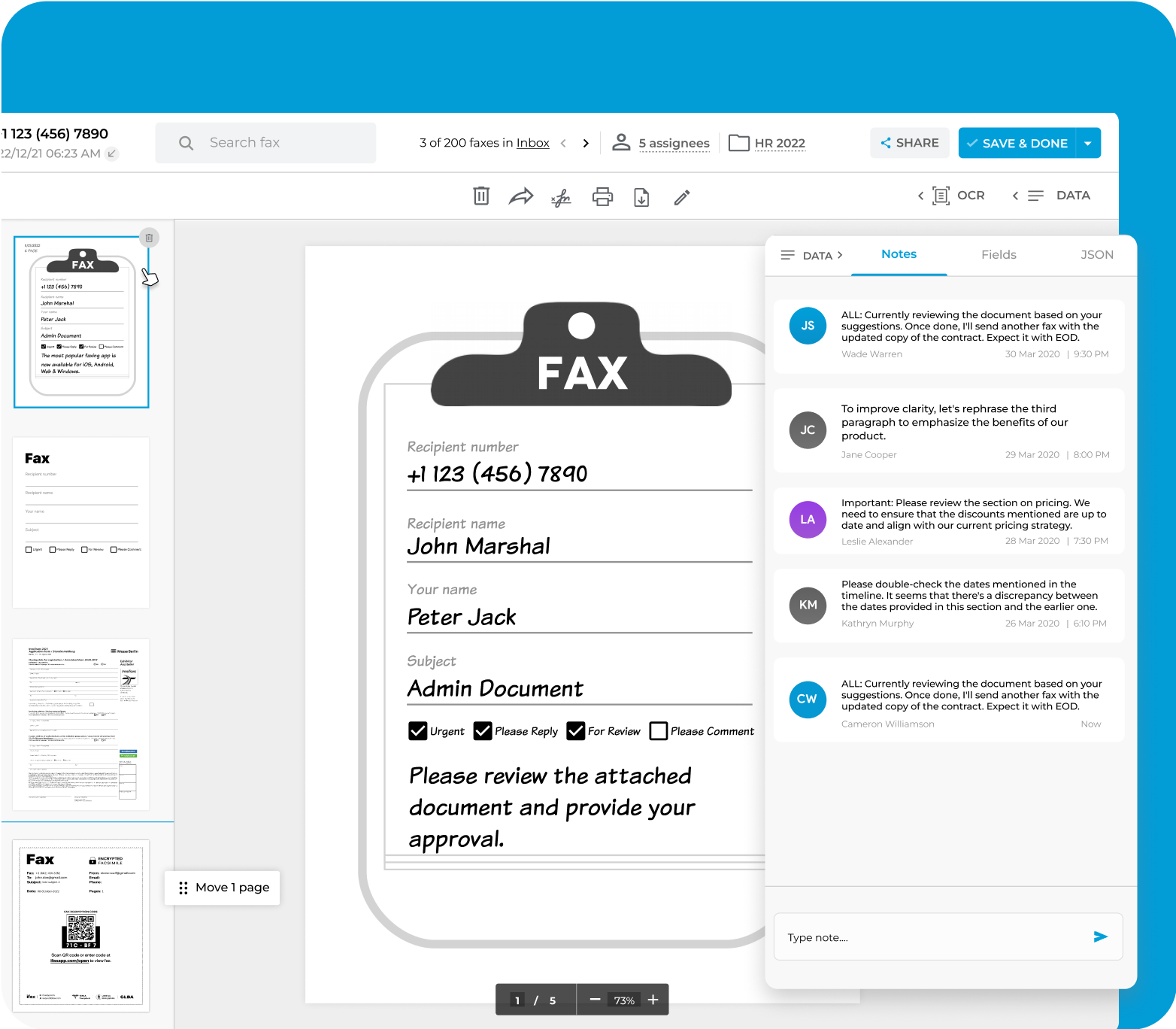
Elevate your document workflow by seamlessly integrating notes into both outgoing and incoming electronic faxes. These notes serve as valuable references, ensuring an organized approach and preventing the oversight of critical details.
Use these notes to prioritize tasks, collaborate with your team on fax documents, monitor document progression, and highlight the status of essential fax-related activities.